
Commercial Denial Statistics
A new study released by Crowe Revenue Cycle Analytics suggests that commercial payers have increased denial claims over the past three years, according to HealthLeaders. The study, entitled "Time for a commercial break," analyzed inpatient and outpatient data from over 1,800 hospitals and 200,000 physicians and found that commercial payors take the longest to pay, require providers to jump through more administrative hoops to get paid, and delay payments to providers via claim denials at a higher frequency than government payors.
Here are some key highlights from the report:
- From 2021 to 2023, the commercial payer percentage of medical necessity inpatient claim denials increased from 2.4 to 3.2%; however, during that same period, the Medicare denial rate remained at 0.2%
- From 2021 to 2023, the commercial payer percentage of inpatient and outpatient claims initially denied for any reason increased from 14.1% to 15.1%, while the Medicare percentages only increased from 3.4% to 3.9%.
- From 2021 to 2023, the RFI denial rate for commercial payers (5.2% to 4.8%) was 12 times greater than the Medicare rate (0.4%).
- Whereas for commercial payers, the percentage of 2023 claims not paid after 90 days for inpatient and outpatient claims was, respectively, 31% and 32%; the Medicare percentages were only 12% and 11%.
SOURCE: ACDIS
ACA, Medicare and Medicaid Denials
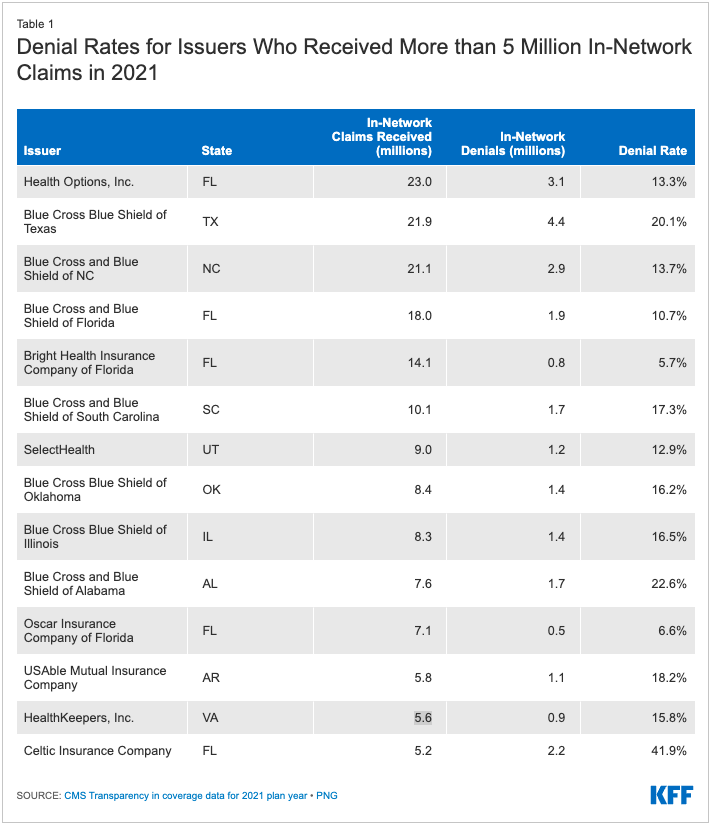
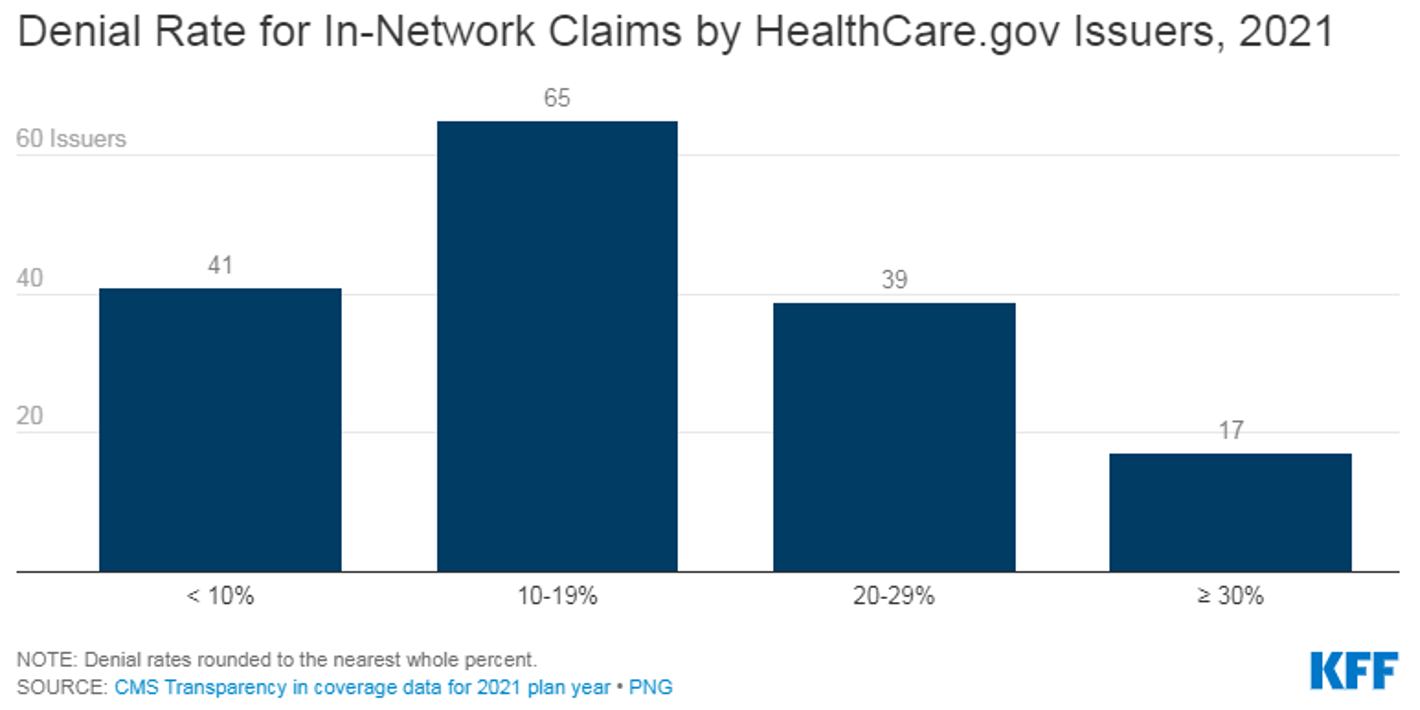
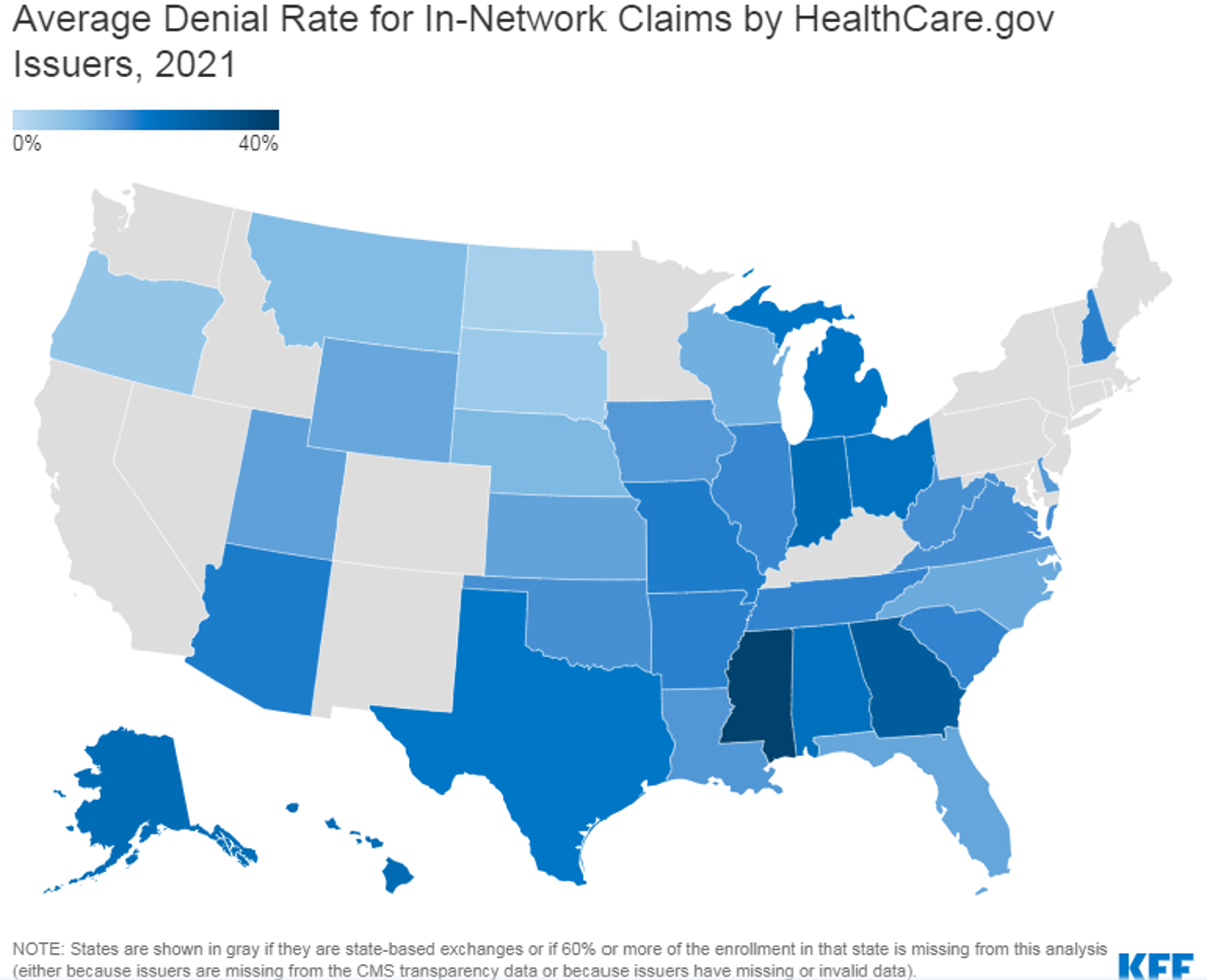
Issuer denial rates for in-network claims ranged from 2% to 49%. In 2021, 41 of the 162 reporting issuers had a denial rate of less than 10%, 65 issuers denied between 10% and 19% of in-network claims, 39 issuers denied 20-29%, and 17 issuers denied 30% or more of in-network claims. (Figure 2) Issuers that report denying one-third or more of all in-network claims in 2021 included Meridian Health Plan of Michigan, Absolute Total Care in South Carolina, Celtic Insurance in 7 states (FL, IL, IN, MO, NH, TN, TX), Ambetter Insurance in 3 states (GA, MS, NC), Optimum Choice in Virginia, Buckeye Community Health Plan in Ohio, Health Net of Arizona, and UnitedHealthcare of Arizona.
Plan-level claims denial data
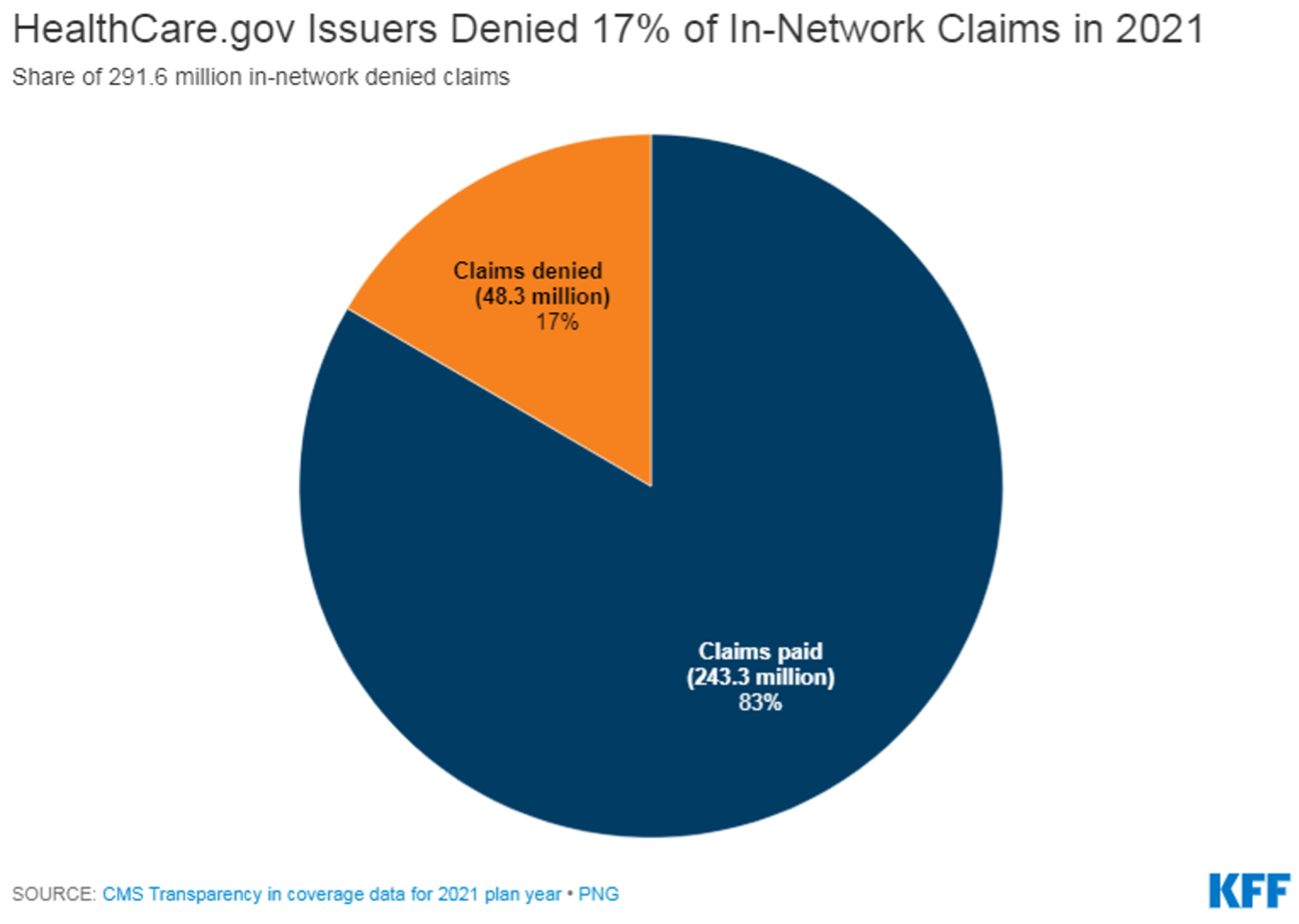
CMS also collects limited transparency data at the plan level. Of the 162 issuers reporting aggregate data, 158 report plan level data on in-network claims received and denied, as well as data on selected reasons for denials. Denial rates varied somewhat based on plan metal levels. On average, in 2021, HealthCare.gov issuers denied 15.9% of in-network claims in their bronze plans, 17.3% in silver plans, 17.1% in gold plans, 11.4% in platinum plans, and 19.7% in catastrophic plans.
Why do health plans deny claims?
HealthCare.gov plans also report on certain categories of reasons for in-network claims denials:
- Denials due to lack of prior authorization or referral
- Denials due to an out-of-network provider
- Denials due to an exclusion of a service
- Denials based on medical necessity (reported separately for behavioral health and other services)
- Denials for all other reasons
A claim might be denied for more than one reason. In addition, insurers are required to report reasons for denials of claims that ultimately are paid. In all, insurers reported 41.7 million denied in-network claims at the plan level for the 2021 coverage year. Insurers also reported 44.7 million reasons for denying in-network claims, including roughly 3 million denials of claims that were later paid.
The distribution of in-network denials by reason is shown in Table 2. (We set aside data for out-of-network claim denials because CMS does not require issuers to report on the number of out-of-network claims received.) About 8% of these 44.7 million denials were for services that lacked prior-authorization or referral, 13.5% were for excluded services, 1.7% for medical necessity reasons, and 76.5% for all other reasons.
Appeals
ACA transparency data show the number of denied in-network claims that consumers appealed to the plan (internal appeals) and the number of denials overturned at internal appeal. Consumers whose denial is upheld at internal appeal sometimes have the right to an independent external appeal. (Under federal regulations, eligibility for external appeal is generally restricted to medical necessity denials, though in some states all denials can be externally appealed.) HealthCare.gov issuers also report the number of external appeals made by consumers, and the number of externally appealed denials that were overturned. The CMS public use file suppresses values lower than 10.
Consumers rarely appeal denied claims. Of the more than 48 million in-network denied claims in 2021, marketplace enrollees appealed 90,599 - an appeal rate of less than two-tenths of one percent. (Figure 4) Issuers upheld 59% of denials that were appealed.
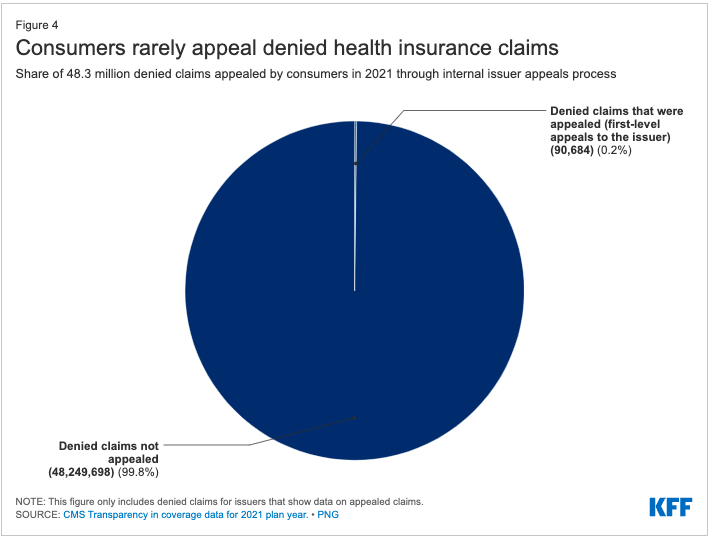
Marketplace consumers also rarely file external appeals. From ACA transparency data (and imputing a value of “5” for each cell where values were suppressed) we estimate just over 2,500 external appeals were filed by marketplace enrollees in 2021.
SOURCE: KFF